Taking your baby’s temperature seems like an easy task, but add on the wiggles and the crankiness (because they’re probably sick!) and it can be pretty difficult! To help you take your baby’s temperature with accuracy, Resident Pediatric RN, Kate Morse is sharing with us how you can take your child’s temperature using digital thermometers rectally, orally, on their forehead, in their ear or under the arm. She’s gotcha covered!! Stay well, everyone!
“I love you so much it hurts!” Have you ever heard this saying? I feel this for my daughter, Ella, every single day. It’s an indescribable, almost gut-wrenching, kind of love. Right? You all know what I’m talking about. You love this person so much and you don’t want to see them sad, hurt, upset, or, worse…. sick.
We’re right in the middle of cold and flu season and it’s pretty inevitable that your little one will come home with some type of viral bug at some point, if they haven’t already. It starts out fairly harmless: a runny nose, and then a cough… and then the fever strikes. Ugh!
If your child isn’t feeling well, it’s always important to check their temperature to see if they have a fever. So let’s chat about a couple of different methods you can use to check your child’s temperature, which methods are most accurate for your little one’s age and what you can do to help them feel better.
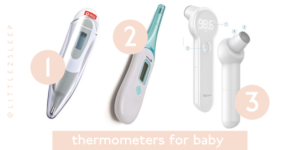
1| $8 Red Cross for rectal, oral & under arm
2| $5 Safety 1st for rectal, oral & under arm
3| $21 Metene for ear and forehead
Digital Thermometers & How To Use
Rectal:
Taking your child’s temperature rectally from birth to 18 months is the most accurate form of measurement. A rectal temperature of 100.4°F (38°C) is considered a fever. If your child is 3 months or younger and has a temperature of 100.4°F (38°C), call your healthcare provider or go to the emergency department right away.
Using a digital thermometer (the Little Z team recommends this one, which also has red lettering making it easy to identify your rectal thermometer from your other thermometers – RED for RECTAL):
- Place your child flat on their back
- Lubricate the thermometer with petroleum jelly
- Lift your child’s legs up as if changing a diaper
- Insert thermometer into your child’s rectum (about ½ inch to 1 inch)
- Wait for the thermometer to beep
- Remove and read temperature
Under the arm (axillary)
You can take your child’s temperature under the arm from age 3 months to 4 years old. An axillary temperature of 99°F (37.2°C) is considered a fever.
Using a digital thermometer (this one can also be used orally):
- Place the thermometer under your child’s arm
- Make sure that the silver tip is touching your child’s skin, not their clothing
- Press their arm firmly towards their body to keep the thermometer in place
- Wait for the thermometer to beep
- Remove and read temperature
Oral
By 4 years of age, your child should be able to hold a thermometer under their tongue. However, some children may show resistance. If this is your child, try explaining that the thermometer is like a straw and all they need to do is hold it in their mouth, as if sipping from a straw. If this does not work, you can revert to taking their temperature under the arm (or using a forehead or ear thermometer). If your child has recently eaten or had something to drink, wait 15 minutes before taking their temperature orally in order to ensure accurate measurement. An oral temperature of 100°F (37.8°C) is considered a fever.
Using a digital thermometer:
- Place the silver tip of the thermometer under your child’s tongue towards the back of their mouth
- Ask your child to close their mouth and cover the thermometer with their lips
- Wait for the thermometer to beep
- Remove and read temperature
Forehead (temporal artery)
A forehead thermometer measures the heat coming from the temporal artery, which is located on the forehead just beneath the skin. This thermometer can be used from 6 months of age and older.
The Little Z team recommends this one, as you can switch out the parts to use as an ear thermometer, too.
- Place the thermometer on the center of your child’s forehead
- Slowly slide the thermometer across their forehead toward the ear while keeping the probe in contact with their skin
- Stop when you reach their hairline
- Remove and read temperature
*Note: some newer models do not require a slide across the forehead. Follow your thermometer’s directions*
Ear (tympanic)
A tympanic thermometer measures the heat coming from the eardrum. This thermometer can be used from 6 months of age and older.
The Little Z team recommends this one, as you can switch out the parts to use as a forehead thermometer, too.
- A correct reading is determined by the placement inside your child’s ear canal. Follow your thermometer’s directions.
- Aim the probe inward, toward the opposite eye and ear
- Keep the probe in place and wait for the thermometer to beep
- Remove and read temperature
Alright, so we know your child has a fever, now what?
Medicine
If your child is fussy, you may give acetaminophen or ibuprofen based on your child’s age and weight.
Do NOT give ibuprofen to a baby less than 6 months old (unless directed by a doctor).
Do NOT give aspirin to a child less than 18 years old (unless directed by a doctor). Reye Syndrome, a rare but sometimes fatal disease, has been associated with aspirin.
If you are unsure of the appropriate dose to give your child, call your healthcare provider to find out. It’s important to note that medicine will not cure the cause of your child’s fever. Medicine provides comfort only. Once the medication wears off, your child’s fever may come back until they are no longer sick.
Lots of Liquids
Be sure to offer your child plenty of fluids to prevent dehydration. Popsicles, ice chips, water, soup and jello are all great options. Try to avoid beverages high in caffeine as this can make dehydration worse.
If your child has vomiting or diarrhea, speak with your healthcare provider about an oral electrolyte solution. Avoid beverages high in sugar as this can prolong diarrhea.
Your child may not feel well enough to eat, so don’t force it. Just ensure they are getting plenty of liquids. Once they feel better, their appetite will return.
Keep it Cool
Have your child wear lightweight clothing, use light sheets or blankets and ensure their bedroom is at a comfortable temperature – not overly warm, and not overly cool.
Rest, rest and more rest
A fever can take it out of your child and cause them to be sleepier than usual. Ensure they are getting adequate rest and relaxation until they begin feeling better. Keep your child home from school or daycare until they have been fever-free (without the use of fever-reducing medication) for 24 hours.
When to Seek Medical Care
Call your healthcare provider if:
- Your child is less than 3 months old with a rectal temperature of 100.4°F (38°C) or higher
- A fever persists for more than 24 hours in a child younger than 2 years of age
- A fever persists for more than 3 days (72 hours) in a child 2 years of age or older
- If your child has any of the following symptoms, in addition to their fever:
-
- Lethargic, sluggish or not acting like themselves
- Not making tears when crying
- Refusing to eat or drink
- Decreased urine output
- Prolonged vomiting or diarrhea
- Develops a rash
- Develops pain with urination
- Has a chronic medical illness
Seek emergency care if your child develops:
- Difficulty breathing
- Blue lips, mouth or nails
- Extreme lethargy and difficulty waking up
- Crying that won’t stop, or extreme irritability
- A sunken or bulging soft spot on infant’s head
- Difficulty moving or walking
- Seizure
- Severe belly pain
- Drooling
- Stiff neck or extreme headache
Here’s hoping your little one stays healthy all cold & flu season long 🙏
Kate Morse
Resident Pediatric RN, BSN
Little Z’s Sleep
*Disclaimer: The content provided by the Little Z team is not intended, nor recommended, to replace medical advice, diagnosis or treatment. Please contact your healthcare provider for medical conditions and questions.*

FLASH SALE
ONE WEEK ONLY
Keep sleep a thing on vacation with the Little Z's Travel Guide!